What is it?
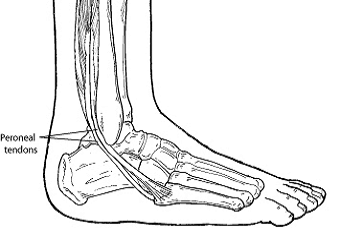 Peroneal tendinopathy is a pathological state of the peroneal tendons or its associated sheath which protects the tendons as it changes course around boney structures. The term tendinopathy refers to a pathological state of a tendon. A tendon may become inflamed, thickened or suffer tears as a consequence of trauma, overuse or a combination of both. There are different stages of tendinopathy relating to the structural form of the tendon. Two common terms used to describe these stages are tendinitis and tendinosis.
Peroneal tendinopathy is a pathological state of the peroneal tendons or its associated sheath which protects the tendons as it changes course around boney structures. The term tendinopathy refers to a pathological state of a tendon. A tendon may become inflamed, thickened or suffer tears as a consequence of trauma, overuse or a combination of both. There are different stages of tendinopathy relating to the structural form of the tendon. Two common terms used to describe these stages are tendinitis and tendinosis.
The peroneal tendons are a group of 3 tendons in the outside of the lower leg which provide dynamic stability to the foot and ankle. The action of the tendons is to evert, or resist inversion of the ankle during activity. The two lateral tendons are most commonly affected by tendinopathy.
How did I get it?
Peroneal tendinopathy may occur as a result of either trauma or overuse. Inversion injury will stretch and potentially tear the tendon if severe. Overuse tendinopathy results from excessive loads to the tendon over time. Improper shoes for your foot shape, poor training programs or decreased strength and proprioception can all contribute to excessive loads. Past injury and laxity to the ligament on the outside of the ankle will additionally cause overload to the tendons. Foot shape also plays a role with overloading the tendon. If the natural shape of your heel is to leave your foot in a rolling out posture then this creates excess force on the tendon.
What does it feel like?
Frequently pain and swelling over the tendon is present as it passes the lateral malleolus (outside bone) of the ankle. This may extend distally to where tendons either attach or curve around the outside of the foot. As in other cases of tendinopathy, pain and swelling are not always present and weakness or instability may be the initial sign that something is not right.
How is it diagnosed?
A description of the area, onset, duration and easing of pain will highlight the potential for peroneal tendinopathy. Palpation along the course of the tendon distal to the ankle bone may be tender. Resisted eversion may elicit pain. Ultrasound and MRI are useful for confirmation of the diagnosis and differentiation of tears in the tendon.
How do I fix it?
- Rest or modification of training programs will allow heeling to take place
- Icing the along the tendon is advantageous regardless of the stage of the condition.
- Orthotic modifications to shoes to unload the tendon are particularly useful in the early stages to reduce pain and swelling.
- Tears frequently are immobilised in a CAM walking boot.
- Stretching of calf muscles can be useful but may be counterproductive during poor tissue quality.
- After the condition improves a slow strengthening program of the tendon/s will aid recovery.
Will I need surgery?
The earlier stages of tendinopathy are successfully managed with conservative treatment. Surgery may be warranted if a longitudinal split is present or if synovitis of the tendon sheath restricts the tendon gliding with ankle movement. Debridement surgery is usually required for fraying or torn tendons to limit the progression of damage and inverted hind foot postures may require realignment surgery.
How do I stop it coming back?
Peroneal tendinopathy can take considerable time to repair. Functional strength programs and footwear and foot structure assessment are important and should be sort before taking up any new activity. Orthotic prescription is particularly beneficial to stabilise the foot and reduce stress on the tendon and realignment surgery for an inverted foot structure if conservative therapy fails.
Peroneal Tendinopathy is one of the conditions we treat at Shore Physio, so please give us a call on 02 9460 6788 to discuss your condition and schedule your session.